What kind of disease prostatitis is, and what the first symptoms it causes, every man should know.Prostatitis is a common urological pathology in which inflammatory processes progress in the prostate gland.The disease is mainly diagnosed in men aged 35–40 years.Predisposing factors that contribute to the onset of the disease are reduced immunity, an inactive lifestyle, abuse of bad habits, and poor nutrition.The diagnosis and treatment of pathology is carried out by a doctor called a urologist.It is with him that you need to make an appointment for a consultation if you are concerned about characteristic symptoms.It is important for any man to remember - the earlier the disease is diagnosed and its treatment is started, the greater the chance of full recovery and recovery.Lack of timely treatment can lead to serious consequences, including male infertility and prostate cancer.
The essence of pathology
Inflammation of the prostate gland is called prostatitis.The prostate is a male organ responsible for producing secretions that maintain normal sperm activity.In most cases, the disease is infectious in nature.Infection can occur through the urethra, blood or lymph flow, when the infection moves throughout the body from distant inflammatory foci.Microorganisms that can provoke an inflammatory complication:
- coli;
- staphylococci;
- enterococci;
- proteas;
- Klebsiella, etc.
All these microscopic organisms are opportunistic microflora, the active life of which is suppressed by the human immune system.But as soon as the immune system is weakened, under the influence of predisposing factors, the infection becomes more active, causing inflammation in the gland tissues.
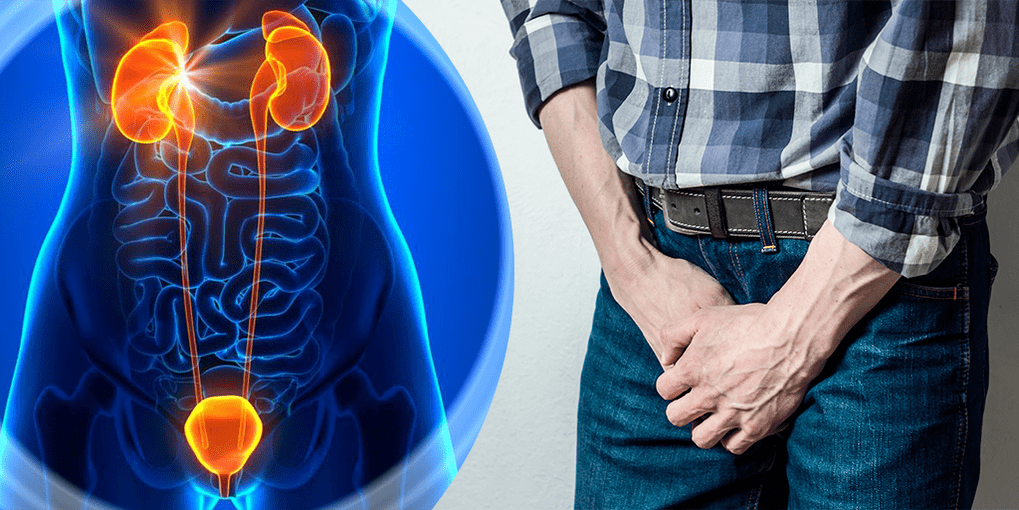
Depending on the nature of the course, the following forms of prostatitis are distinguished:
- acute;
- chronic.
Acute is characterized by pronounced symptoms; with timely seeking medical help, it can be successfully cured.The chronic type of pathology occurs as a result of inadequate or untimely treatment of the acute form.The disease is characterized by recurrent infection, which manifests itself with vague symptoms.Chronic prostatitis cannot be completely cured, but properly selected therapy and preventive measures help prolong remission.
Reasons
The key causes of prostatitis are decreased immunity, untreated urological and venereal infections.Inflammation often occurs against the background of a bacterial infection, which, with the proper functioning of the immune system, is in a latent state.But as soon as the immune system weakens, pathogens become more active, causing inflammation of the prostate tissue.
What causes prostatitis:
- Hypothermia.Hypothermia causes stress in the body, promotes vasospasm, poor circulation, and decreased immunity.
- Inactive lifestyle.With a sedentary lifestyle, the blood supply to the pelvic organs deteriorates, which leads to stagnation and the development of inflammation in them.
- Chronic constipation.Hardened feces, which lie in the intestines for a long time, put pressure on the gland, disrupting microcirculation.This creates favorable conditions for the life of pathogenic microflora.
- Injuries.Traumatic damage to the prostate contributes to a deterioration in blood flow and a decrease in local immunity.
- Excess body weight.People who are overweight move little, which causes blood circulation in their internal organs to deteriorate.Stagnant processes lead to swelling and inflammation of the prostate tissue.
- Disturbance of the rhythm of sexual activity.Prostatitis can be caused by both an overly active sex life and prolonged abstinence.
- The presence of chronic pathologies.Any source of chronic infection can be potentially dangerous for the prostate and can cause inflammation.
- Conditions that contribute to the suppression of the immune system.The general condition of the body is negatively affected by chronic stress, overwork, regular lack of sleep, and physical overload.
Types of prostatitis
Symptoms of prostatitis depend on its type and nature of the course.There are several types of the disease, each with its own characteristics.
Bacterial
The main cause is a bacterial infection that develops against a background of weakened immunity.Bacterial prostatitis occurs:
- spicy;
- chronic.
In acute cases, pronounced prostatitis syndromes are of concern:
- a sharp increase in temperature;
- urinary disturbance;
- pain, discomfort in the perineum;
- purulent, bloody inclusions in the urine;
- deterioration in general health.
In a chronic course, the symptoms are blurred and appear weakly.But in case of relapse, the intensity of the symptoms resembles an acute process.
Calculous
This type of pathology is mainly diagnosed in men over 55 years of age.An inflammatory complication develops against the background of the formation of stones in the prostate tissue.Most often, stones are formed due to improper treatment of chronic prostatitis.Another common root cause is untreated urolithiasis.
Characteristic signs of calculous prostatitis:
- urinary disturbance;
- hematuria;
- weakening of erection.
Stagnant
It develops against the background of chronic prostatitis and is associated with impaired microcirculation in the pelvic organs.Also, the stagnant form can occur with a long absence of sexual intercourse, which leads to stagnation of secretions in the gland.
Characteristic symptoms of congestive prostatitis:
- problems with urination;
- discomfort in the groin and testicles;
- erectile dysfunction.
Purulent
Purulent prostatitis develops against the background of an acute form of the disease, the treatment of which is incorrect or completely absent.The pathology is characterized by a significant increase in body temperature, impaired urination, the presence of purulent inclusions in the urine, and acute pain in the groin and perineum.If treatment is not started immediately, there is a high probability of developing an abscess and blood poisoning, which can lead to the death of the patient.
Symptoms
Symptoms and treatment of prostatitis depend on the stage of its progression:
- Catarrhal.At this stage, the patient complains of frequent urination, pain when going to the toilet, discomfort in the perineum during physical activity.
- Follicular.The pain symptom becomes more pronounced, bothers you even at rest, and can radiate to the lower abdomen or lower back.The process of urination is disrupted, liquid flows out in a thin stream, and sometimes urinary retention occurs.
- Parenchymatous.An advanced stage, during which general intoxication of the body develops, body temperature rises significantly, unbearable pain in the perineum occurs, and problems with urination become more pronounced.
Pain syndrome
There are no pain receptors in the prostate, but pain occurs due to an increase in the size of the gland and irritation of nearby nerve fibers.The more advanced the disease, the more severe the pain that worries the person.The pain syndrome can change intensity with sexual abstinence or increased sexual activity.Discomfort spreads to the lower abdomen, lumbar region, perineum, and scrotum.
Dysuric syndrome
When inflamed, the prostate increases in size and begins to put pressure on the ureters, which is why their lumen gradually decreases.The patient begins to be bothered by frequent urination, and after visiting the restroom there remains a feeling of incomplete emptying of the bladder.
Sexual deviations
In the initial stages of development of the pathology, a man may be bothered by frequent erections or, conversely, a lack of sexual arousal.Accelerated ejaculation is explained by a decrease in the sensitivity threshold of the excitation center.If treatment for prostatitis is not started at the initial stages, complications develop that lead to impotence and infertility.
Diagnostics
If you have characteristic symptoms, you should consult a doctor.Diagnosis and treatment of prostatitis is carried out by a urologist.It is with him that a man should make an initial appointment.During the examination, the doctor will ask about disturbing symptoms, complaints, collect anamnesis, and conduct a rectal examination of the prostate gland.To confirm the diagnosis, the urologist will give a referral for additional diagnostic examination, including the following procedures:
- clinical blood and urine analysis;
- PCR research;
- uroflowmetry;
- examination of gland secretions;
- Ultrasound of the prostate;
- CT or MRI.
Treatment
The treatment regimen is determined taking into account the nature of the course and the degree of neglect of the pathology.If the patient's condition is serious, the doctor decides on hospitalization.Otherwise, treatment is carried out on an outpatient basis.The patient must strictly follow the urologist’s instructions, adhere to the treatment plan and not self-medicate.
Drug therapy
Antibiotics will help stop the inflammatory process and destroy pathogenic microflora.If prostatitis is caused by viruses or fungi, the antibacterial treatment regimen is supplemented with appropriate groups of drugs.
To eliminate pathological symptoms, the following groups of drugs are additionally prescribed:
- non-steroidal anti-inflammatory drugs;
- painkillers;
- muscle relaxants;
- antispasmodics;
- alpha-blockers;
- diuretics;
- drugs that normalize prostate function.
If a man complains of problems with potency and sexual dysfunction, the doctor prescribes drugs that stimulate blood circulation in the penis and restore erection.
Maintenance therapy
The effect of drug therapy will be enhanced by supportive measures, including the following rules:
- Drink the required amount of fluid - at least 1.5 - 2 liters per day.
- Maintaining bed rest.
- Warm therapeutic baths.
- Following a gentle diet, during which salty, spicy, fatty foods, alcohol, coffee, and sour drinks are excluded from the diet.
The patient's condition is favorably influenced by regular sex life, which ensures drainage of the prostate and prevents stagnation of secretions.
Surgical intervention
If conservative treatment does not bring the desired effect, the doctor decides to perform surgery.In modern urology, the following surgical methods for treating prostatitis are practiced:
- Transurethral resection (TUR).During the operation, the surgeon removes all affected gland tissue.
- Prostatectomy.Involves removal of the prostate, adjacent tissues, and seminal vesicles.
Surgery is not performed on young men because any operation can cause infertility.
Folk remedies
In addition to complex drug therapy, alternative medicine can be used.The treatment regimen must be agreed with the doctor.Self-medication is unacceptable.
To combat inflammation and disturbing symptoms, medicinal herbs rich in beneficial substances and elements that have a bactericidal and anti-inflammatory effect are used.Based on medicinal herbs, infusions, tinctures, and decoctions are prepared, which can be taken orally, made into compresses and lotions, and added to the bath.
The following herbs are used to treat prostatitis:
- sage;
- calendula;
- chamomile;
- licorice;
- yarrow;
- nettle;
- parsley;
- St. John's wort;
- bearberry;
- rosemary;
- centaury;
- ginseng;
- sweet clover;
- chestnut.
For chronic prostatitis, bee propolis is widely used, which is famous for its anti-inflammatory properties and analgesic effect.Adherents of alternative medicine advise making suppositories from propolis, which are inserted into the rectum.The recipe is:
- Grind 20 g of propolis to a powder.
- Combine the main component with 200 ml of alcohol and evaporate over low heat.
- Add 2 g of cocoa butter to the resulting mass.
- Form a candle from the finished composition.
- The product is inserted into the rectum overnight.Treatment is carried out in a course and lasts 1 month.
Consequences
Lack of proper treatment or self-medication can result in serious health problems.The spread of infection leads to the development of such negative consequences as:
- cystitis;
- pyelonephritis;
- vesiculitis;
- colliculitis and urethritis;
- epididymitis;
- prostate sclerosis.
Against the background of such complications, erectile and psychological disorders occur.In severe cases, the disease can progress to the stage of chronic calculous prostatitis, causing an abscess and other life-threatening complications.Frequent relapses often cause the development of male infertility, adenoma and even prostate cancer.
Prevention
Preventing prostatitis is much easier than fighting the disease and its consequences.The following simple and affordable preventive measures will help prevent inflammation of the prostate or prolong remission in the chronic form:
- active lifestyle;
- control of proper nutrition and water regime;
- eliminating bad habits;
- elimination of stress factors;
- hardening;
- maintaining basic personal hygiene;
- normalization of body weight;
- timely and adequate treatment of infectious pathologies;
- regular, high-quality, protected sex;
- annual preventive visits to the urologist.





























